Painful Sex After Hysterectomy: Why It Happens and What Can Help
Pain during sex after a hysterectomy is more common than many people expect. While a hysterectomy is often done to improve quality of life, some individuals notice new pain with vaginal intercourse after surgery or find that the pain they already had does not fully go away.
This can feel confusing, especially if there was an expectation that sex would feel better after surgery. Pain with intercourse, called dyspareunia, is not something to ignore or push through. Understanding why it happens can make it easier to find solutions that actually help.
In this blog post, you'll learn more about why painful sex can occur after a hysterectomy, as well as the most effective treatment options for relief.
How Common Is Painful Sex After Hysterectomy?
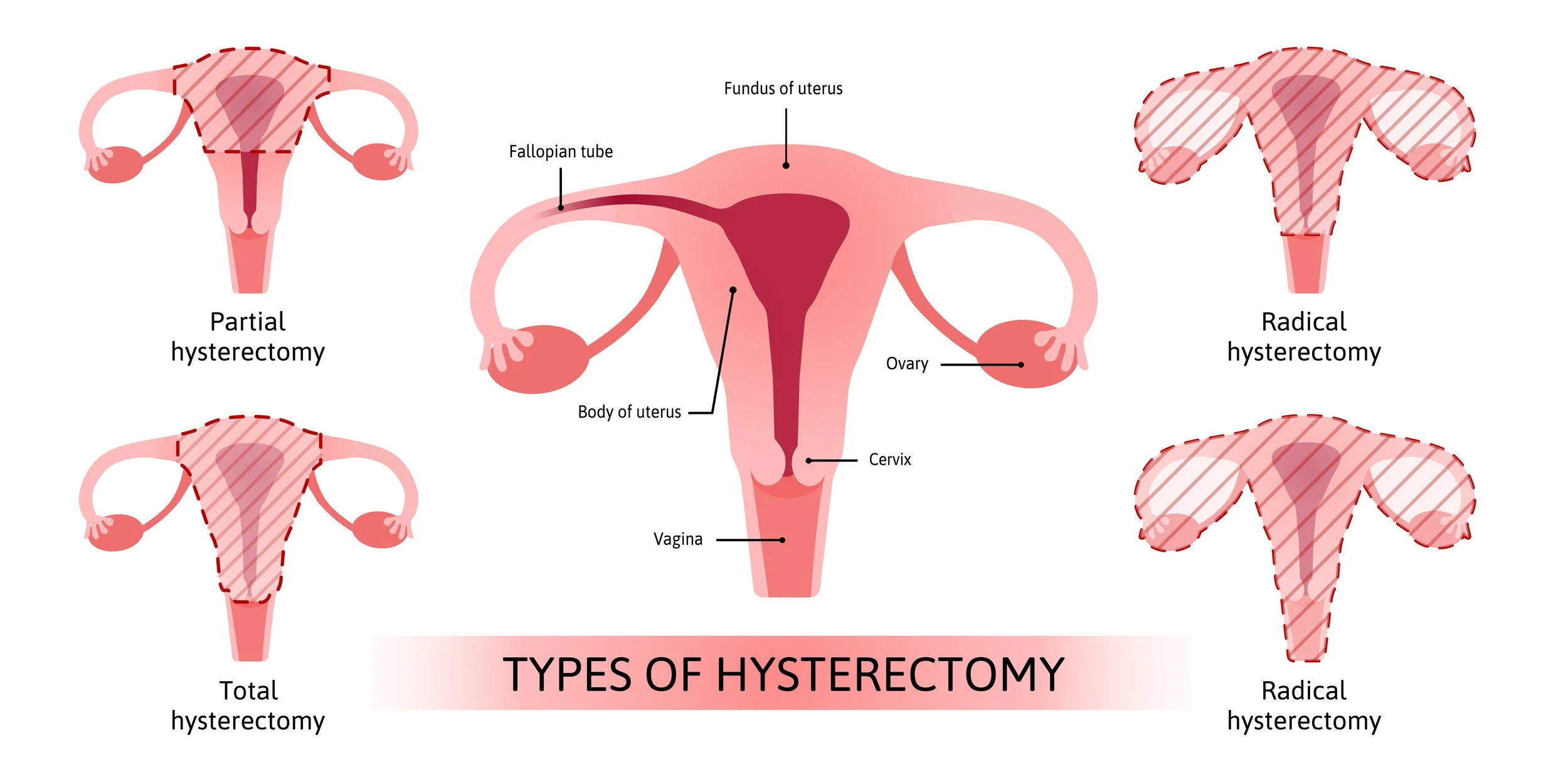
It’s not unusual for people to experience changes in sexual comfort after a hysterectomy. After all, a hysterectomy involves removing the uterus, and in some cases, the ovaries and the top portion of the vagina. These structures are involved not only in childbearing but also in hormone production and sexual function.
While many people report improvement in painful vaginal intercourse if they had pain prior to hysterectomy, others notice new or ongoing pain with penetration. Most individuals experience an improvement in sexual pain after surgery. However, studies suggest that about 4–19% of people continue to experience persistent pain with sex after hysterectomy.
It’s important to remember that painful sex after a hysterectomy does not mean something went wrong with the surgery. In many cases, pain is related to changes in muscles, tissue flexibility, hormones, or how the body responds to touch after healing.
Why Sex Can Be Painful After Hysterectomy
Pain with sex after a hysterectomy usually has more than one cause. Short-term healing changes and longer-term body changes can both play a role.
Short-Term Reasons
In the months after surgery, pain may be linked to normal healing.
The area at the top of the vagina, called the vaginal cuff, can remain sensitive for a period of time.
Pelvic floor muscles may tighten to protect the vaginal and pelvic floor area, which can make penetration uncomfortable.
Scar tissue is also forming during this time, and can be sensitive during healing.
Long-Term Reasons
Changes in vaginal depth or flexibility
After a hysterectomy, the vaginal canal may be slightly shorter or less flexible. This can make deeper penetration uncomfortable due to reduced vaginal length or tension at the vaginal cuff.
Pelvic floor muscle tension or poor coordination
Pelvic floor muscles play an important role in relaxation and comfort during sex. If these muscles stay tight or do not relax fully, penetration can feel painful or restricted.
Scar tissue tightness
Internal scar tissue can limit tissue mobility and cause pulling, burning, or sharp pain during sex.
Hormonal changes and low estrogen
If the ovaries are removed or if menopause occurs around the time of surgery, estrogen levels decrease. Low estrogen can make vaginal tissue thinner, drier, and more sensitive. This group of changes is often referred to as genitourinary syndrome of menopause (GSM), which is a common contributor to pain with sex after hysterectomy.
Decreased arousal
With decreased arousal or desire, there may be less natural lubrication and blood flow to the vaginal tissues, as well as reduced flexibility of the pelvic floor muscles and vagina, which can increase discomfort with penetration.
What Can Help Painful Sex After Hysterectomy
Pain with sex after a hysterectomy is treatable, and many people experience improvement with the right combination of support and care.
Pelvic Health Physical Therapy
Pelvic health physical therapy (also called pelvic floor rehabilitation) is one of the most effective treatments for pain with sex. Treatment may include:
Retraining pelvic floor muscles to relax
Addressing scar tissue sensitivity and mobility
Reducing fear or muscle guarding around penetration
Education on lubricants, vaginal moisturizers, and pain-reduction strategies
To learn more about what to expect in pelvic floor physical therapy, watch my YouTube video, “What to Expect in Pelvic Floor Therapy”, for guidance on what pelvic PT involves and how to find a pelvic health provider near you.
Depth Control and Position Changes
If pain occurs mainly with deeper penetration, limiting depth can help. Devices like the Ohnut allow partners to control how deep penetration goes, which can reduce pain while still allowing intimacy. Changing positions can also make a difference. For example, positions where the person receiving penetration controls depth and angle often feel more comfortable.
Lubricants and Vaginal Moisturizers
Dryness is a common reason for pain after a hysterectomy, especially with hormonal changes. Using a high-quality moisturizer and help with discomfort from dryness, and lubricant can reduce friction and irritation. But not all lubricants are the same, and some can worsen irritation. Learn more and watch my YouTube video, “What You Need To Know About Lubricants”.
Vaginal Estrogen
Low-dose vaginal estrogen can improve tissue moisture, thickness, and comfort for people with low estrogen levels, particularly those experiencing GSM. Discuss this option with a medical provider to determine whether it is appropriate for you.
Gradual Return to Penetration
Pain can lead to fear or muscle tightening, which may increase discomfort over time. Gradually returning to penetration, with guidance and support, can help the body relearn relaxation and comfort. In addition to working with a pelvic health physical therapist, some people find it helpful to work with a counselor — especially an AASECT sex therapist.
When to Seek Help
Pain with sex is not something you need to live with. Support may be helpful if:
Pain lasts beyond the expected healing period
Pain feels sharp, burning, or worsening
Fear or avoidance of intimacy develops
Lubricants or position changes alone are not enough
Painful sex after a hysterectomy can feel isolating, but comprehensive and compassionate care is available.
Personalized, One-on-One Support in Jacksonville, Florida
At OncoPelvic PT, Dr. Alex Hill, PT, DPT, OnCS, PWCS, CLT-LANA, provides comprehensive pelvic health care for people experiencing pain with sex, including after a hysterectomy, through in-clinic and virtual visits. Care focuses on education, evidence-based treatment, and helping people return to intimacy comfortably and confidently.
You can learn more or schedule an evaluation here:
https://www.oncopelvicpt.com/services