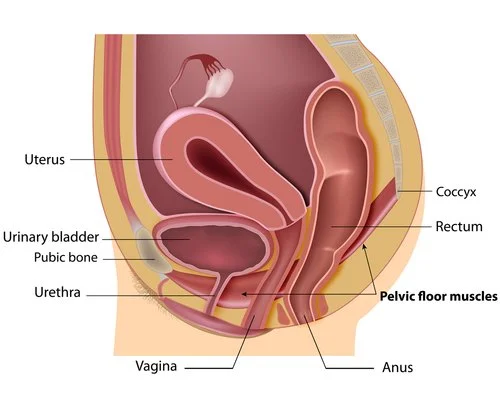
Pelvic Floor Weakness After Childbirth: 5 Evidence-Based Interventions That Work (Beyond Kegels)
Symptoms due to pelvic floor weakness after childbirth is very common – but that doesn’t mean you can’t do something about it! Many people notice bladder leaks, pelvic pressure, difficulty returning to exercise, or a feeling that their core does not work the same way it did before pregnancy. Not only are these symptoms bothersome right after delivery, but they often persist well beyond the early postpartum weeks.
Despite how common these concerns are, many postpartum individuals are still given limited guidance - often to “just do Kegels” or to wait it out. While pelvic floor exercises can be helpful, they are usually not enough on their own.
Pelvic floor recovery after childbirth involves more than just the pelvic floor muscles. It requires coordination, strength, breathing, and movement patterns working together. This blog post covers five evidence-based approaches that help improve pelvic floor function after childbirth, going beyond Kegels alone.
What Pelvic Floor Weakness After Childbirth Really Means
Pelvic floor dysfunction does not always mean the muscles are simply weak. In many cases, the muscles may not work at the right time, may not relax fully, or may not coordinate well with the rest of the body
During pregnancy and childbirth, the pelvic floor supports increased weight and pressure. Hormonal changes affect connective tissue, abdominal muscles stretch, and the pelvic floor works harder to support the growing uterus. Additionally, birth itself can place stress on muscles, nerves, and connective tissue. Postpartum recovery then occurs during a time when sleep is limited and daily physical demands are high, especially while caring for a newborn, which can contribute to ongoing pelvic floor symptoms.
Common postpartum pelvic floor symptoms include leakage with coughing or exercise, pelvic heaviness or pressure, back or pelvic pain, and difficulty returning to activities such as running or strength training. These symptoms signal that the pelvic floor needs comprehensive support and retraining.
Why Kegels Alone Often Do Not Fix the Problem
Kegels are repeated contractions of the pelvic floor muscles, similar to strengthening any other muscle group. While this can be helpful for some people, it does not address all aspects of pelvic floor function.
The pelvic floor needs to work automatically during daily activities such as lifting, standing, and exercising. If the muscles are not timed well with movement and breathing, symptoms like leakage can continue even with regular Kegels.
On the other hand, some individuals struggle to fully relax the pelvic floor muscles; tightness or overactivity can cause symptoms just as much as weakness. Additionally, the pelvic floor relies on support from the abdominal muscles, hips, and glutes. If those areas are weak or not working well, the pelvic floor may take on more load than it can manage, leading to symptoms.
Five Approaches That Support Postpartum Pelvic Floor Recovery
Pelvic Floor Coordination and Control
Pelvic floor recovery starts with learning how the muscles function during real-life movements. This includes coordinating pelvic floor activity with breathing and movement, rather than only squeezing while lying or sitting still.
Training may focus on pelvic floor activation during tasks like coughing, standing up, lifting, or carrying. Learning how to fully relax the muscles is equally important because improved coordination often leads to symptom improvement before more traditional strengthening begins.
If you need help learning how to perform pelvic floor exercises correctly, my YouTube video below walks you through how to contract, relax, and isolate the pelvic floor muscles effectively.
Biofeedback When Needed
Biofeedback is a tool that helps people better understand how their pelvic floor muscles function and can be helpful during postpartum recovery. One form of biofeedback uses sensors placed at the pelvic floor to send information to a computer, showing when the muscles are contracting or relaxing.
Biofeedback is most helpful when it is difficult to sense what the pelvic floor is doing. Not everyone needs it, but it can support learning and confidence when awareness is limited.
Strengthening the Core
The pelvic floor works as part of a team with the abdominal, back, hip, and glute muscles, which together help support the body during movement. Strengthening these areas improves support for the pelvic floor during daily activities and exercise.
Postpartum rehabilitation often includes exercises that build strength while teaching these muscles to work together. This helps reduce strain on the pelvic floor and supports a safer return to activity. For guided exercise routines that focus on early core strengthening, visit my Pregnancy and Postpartum YouTube playlist.
Breathing and Pressure Management
Breathing plays a significant role in pelvic floor health. Frequently holding your breath or pushing downward during effort, such as straining for bowel movements or lifting heavy items, increases pressure on the pelvic floor.
Learning how to breathe during movement, especially exhaling during effort, while optimizing posture and body mechanics, can help support the pelvic floor. These strategies assist with pressure control during lifting, exercise, and daily tasks to reduce symptoms.
Lifestyle and Movement Changes
Daily habits influence pelvic floor recovery. Constipation, inadequate hydration, and straining increase stress on the pelvic floor. Lifestyle changes including improving bowel habits or gradually progressing back to higher-impact activities, support healing while muscle strength, endurance, and coordination improve. These strategies are meant to help recovery, not limit long-term activity.
Need help with constipation? I’ve created an entire YouTube bowel playlist to help you keep things moving smoothly without straining or stressing your pelvic floor.
What Postpartum Pelvic Floor Rehabilitation Should Include
It is becoming more common for postpartum individuals to work with a pelvic floor physical therapist, and research suggests that rehabilitation support improves postpartum recovery outcomes. Effective pelvic floor rehab is personalized, comprehensive, and guided by individual goals.
Postpartum rehab considers how the body moves, how breathing and pressure are managed, and what activities are most meaningful. Sessions can include education, movement retraining, and exercises that reflect real-life demands. Care should not rely solely on endless Kegels, biofeedback alone, or fear-based restrictions. Progress should feel gradual, supportive, and empowering.
Pelvic floor weakness and related symptoms after childbirth are common, but they do not have to be permanent or managed with Kegels alone. Recovery is often most successful when it starts early and takes a full-body approach.
Postpartum Pelvic Floor Therapy in Jacksonville, Florida
If you are experiencing bladder leaks, pelvic pressure, core weakness, or difficulty returning to exercise after childbirth, working with a pelvic floor physical therapist can help.
At OncoPelvic PT in Jacksonville, Florida, Dr. Alex Hill, PT, DPT, OnCS, WCS, CLT-LANA, provides personalized, evidence-informed postpartum pelvic health care through in-clinic, mobile, and virtual visits. With over 12 years of experience and dual board certification in Women’s & Pelvic Health and Oncology, Dr. Alex specializes in comprehensive pelvic floor rehabilitation that goes beyond Kegels alone.
Each evaluation is tailored to your goals, movement patterns, and symptoms to support a confident return to exercise and daily activities.
You can learn more or schedule an evaluation here:
https://www.oncopelvicpt.com/services